We probably don’t need to tell you this, but pregnancy and childbirth certainly take a toll on your pelvic floor muscles. Yet, when we talk about postpartum “core recovery,” most people think primarily about their abdominal muscles. While your abs are certainly important, we cannot ignore the “floor of your core” — your pelvic floor. The pelvic floor muscles are perhaps the most neglected group of muscles in the body, but they are critical core muscles that have very important functions. Given the stress these muscles undergo during pregnancy and childbirth, proper recovery work is essential to build a strong and functional core. But no, it’s not about “just doing Kegels” as we so often hear.
Understanding Your Pelvic Floor
Let’s begin by understanding a bit more about the structure and function of your pelvic floor muscles. There are 14 pelvic floor muscles in total. They form a sling at the bottom of your core.
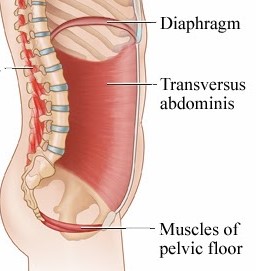
Many people think of their pelvic floor muscles as just those “pee-stopping” muscles, but actually that is just the front of your pelvic floor. As you can see in the image below, the pelvic floor muscles have connection points in the front, back, and sides of your pelvis.
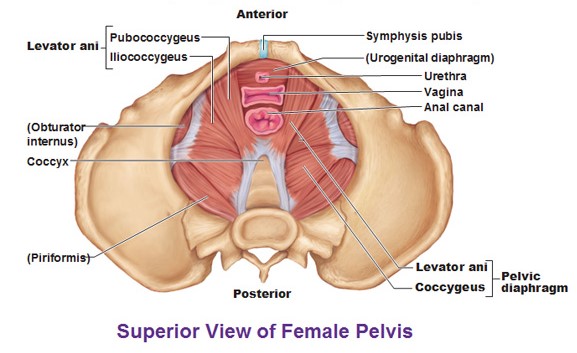
Together, the pelvic floor muscles are responsible for:
- Supporting your pelvic organs: uterus, bladder, rectum
- Helping to stabilize your spine and pelvic-hip region
- Controlling continence (making sure you pee when you want to, and don’t pee when you don’t want to)
- Aiding in sexual response and satisfaction
- Assisting in guiding the baby out during delivery
How Pregnancy Impacts Your Pelvic Floor
During pregnancy, the pelvic floor muscles are stressed with the added weight of your growing belly and uterus. In addition, the common pregnancy alignment shifts — especially the anterior tilt (or low back arch) caused by the growing belly — can accentuate pressure on these muscles.
Then, comes the added trauma of childbirth. In a vaginal birth, the pelvic floor muscles are responsible for helping to guide the baby out during delivery. However, if these muscles are weak or underactive, this could result in increased tearing. A C-section also traumatizes the pelvic floor muscles. During the procedure, the abdominal muscles are moved in order to pull the baby out. Because of how intricately connected the abdominal and pelvic floor muscles are, this major abdominal surgery also impacts the pelvic floor.
So, in summary, pregnancy alone puts a great deal of excess strain on the pelvic floor muscles. However, delivery certainly adds to it, and that’s why pelvic floor dysfunction is more common in the postpartum period.
Pelvic Floor Recovery Work
You can begin pelvic floor recovery work as soon as you feel comfortable following delivery. In fact, some studies show that gentle pelvic floor activations done within the first 24 hours after delivery can help increase blood flow to the area to expedite healing. Of course, depending on your delivery experience, let comfort be your guide.
When it comes to specific pelvic floor exercises, we teach exercises called PFAs (Pelvic Floor Activations). We do not use the term “Kegel” because these exercises have become synonymous with “squeezing the muscles used to stop the flow of urine.” There are two issues with this description:
- Your “pee-stopping” muscles are only the front of your pelvic floor (this misses the back and sides).
- A focus on the contraction only can cause your pelvic floor muscles to go into a shortened (overly tight) state, which can actually lead to, or exacerbate, pelvic floor dysfunction. Like all other muscles in your body, your pelvic floor muscles must be worked through a full range of motion, which requires being able to lengthen them.
There are two variations of this — PFAs Slow and PFAs Fast. Watch the video below for a step-by-step guide that shows you how to first find your pelvic floor muscles and then teaches you how to perform the PFAs.
PFA Recap
Let’s review the key takeaways from the video:
- Find your pelvic floor muscles: front, back, and sides
- Practice moving them together (lifting up, then fully releasing)
- Align this movement with your 360˚ Breathing. This is a PFA-Slow
- Continue this same motion, but at a slightly faster tempo, not aligned with your breath (just breathe comfortably). This is a PFA-Fast.
- Practice both PFAs-Slow and PFAs-Fast, as they target different muscles fibers.
Expert Tip
One great way to get in your pelvic floor work is to align your PFA practice with an activity that you do daily to help you establish a habit. This way, your practice becomes routine — something you don’t have to try to remember (because remembering to shower and brush your teeth is challenging enough in the early postpartum days). For new moms who are nursing or bottle feeding, we recommend practicing your PFAs every time you sit down to feed your baby. Aligning your pelvic floor work with an activity like feeding your baby ensures you get in plenty of practice!
In terms of reps and sets, there is no specific rule on this. As one example, you could say 1 set = 3-5 PFAs-Slow + 8-10 PFAs Fast. Perform 2-3 sets at every feeding session.
Want Additional Resources?
For additional resources to help you recover, build strength, and get back to doing what you love, explore our Postpartum Training Programs. Or, for a more personalized approach, visit our Find a Coach page to find an expert trainer who can design and coach you through a customized training program.
Are you a Health & Fitness Professional?
If you are a health & fitness professional interested in coaching pre & postnatal clients, explore our ProNatal Education & Certification.
