Giving birth, no matter how it happens, is a life-changing experience. It’s important to realize there is no hierarchy of birth outcomes. While you might be surrounded by people who place vaginal birth on a pedestal – there are so many nuances, and so much unpredictability when it comes to birth stories that we are not able to say that one type of birth is “better” or “worse” than another.
That said, A Cesarean birth is major abdominal surgery, and we want to make sure you have the information you need to heal your body afterward — especially since this information is not often provided after the procedure. Unfortunately, when we compare a C-section with other major surgeries (like hip, knee, or shoulder), it’s shocking to see the difference in post-operatives procedure or guidance. For most orthopedic surgeries, there is a regimented rehabilitation process, which includes physical therapy. For a C-section, you’re pretty much given your baby, perhaps told to rest and not lift anything heavy, and bid “good luck.”
In this piece, we hope to fill some of the gaps in guidance and get you started strong on your path to recovery.
What Happens During the Procedure?
Let’s begin by understanding the procedure itself. An uncomplicated cesarean birth is a fairly quick experience, averaging about 45 minutes in duration. Though, you’ll meet your baby in the first 10 to 15 minutes. Once you’re in an operating room, an anesthesiologist – in collaboration with your obstetrician – will anesthetize you from the waist down so that you can remain awake (as opposed to general anesthesia, during which you would be asleep).
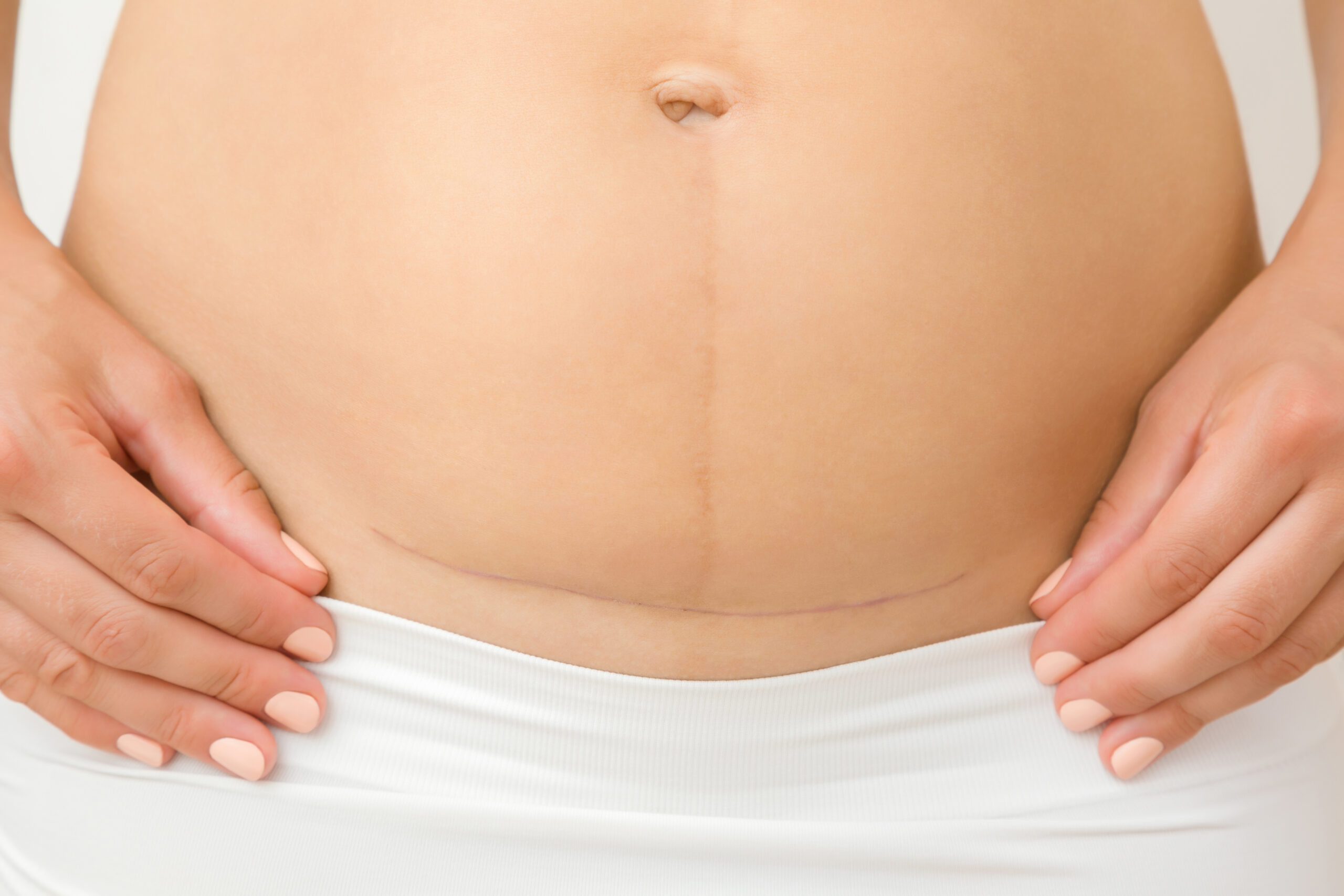
Your obstetrician most often makes a horizontal incision at your bikini line – as is shown in the photo below – through the skin, fat, and fascia into the uterus to remove the baby and placenta. Your abdominal muscles are moved during this procedure, not cut.
It’s important to know that the epidural (or spinal anesthesia) removes pain, but does not remove pressure. So, it’s important to be prepared for the sensation of “tugging” and discomfort. To help you through this, you can prepare some coping strategies like deep breathing, affirmations, head massage from a partner or a doula, or even using music or aromatherapy to increase your feeling of safety and overall satisfaction with your birth. Once your baby is out, the stitching of several layers of tissue begins. This takes most of the time, but hopefully you have a beautiful distraction. Y
How Your Body Changes After a Cesarean Birth
Obviously, the procedure greatly impacts the abdominal muscles. You might think that because this is not a vaginal birth, the pelvic floor is not affected. However, because the abdominal and pelvic floor muscles are so intricately connected, moving abdominal muscle greatly impacts the pelvic floor as well.
In addition, the cutting and stitching of tissues causes some disruption in the neuro-sensory system. For example, many individuals experience nerve changes, including a loss of feeling at the incision site for some time until the nerves regenerate (although sometimes the sensation never fully returns). Many often describe feeling “disconnected” from their core, and not being able to recruit their muscles properly.
Finally, the C-section scar can lead to adhesions below the surface of the skin, making it more difficult for the tissues to move. This could cause pain or sensitivity around the scar, or a feeling of stiffness or movement restriction (making bending forward, lifting, or reaching upward uncomfortable). It could also lead to incontinence, pelvic or low back pain, and other core-related issues.
This is why core and pelvic floor recovery work, along with scar mobilization, is so important. Let’s discuss this more in detail.
Effective Recovery Strategies
Now that you have a picture of the disruption that a C-section can cause, let’s talk about solutions for effective recovery. You can apply these strategies at any point of your post-surgery recovery. Of course, the sooner you start, the better.
- Mental check-in
If you had an unplanned or emergency Cesarean, you may be dealing with some negative feelings about your birth experience. We’ve heard statements from people saying they felt like a “failure” because they did all the right things and trained so hard for a vaginal birth.It is important to remember that there are so many factors outside of your control during labor. Perhaps the process did not go as planned, but resiliency is a hallmark trait of great athletes, and letting go of any negative feelings can actually expedite your healing process. Research shows that a positive mindset is linked to faster healing after injury/surgery (Broadbent and Koschwanez, 2012). - Move in Neutral Alignment
While this strategy might seem tough in the early postpartum (sleepless) days, try as much as possible to move your body in Neutral Alignment (maintaining a straight line between your ear-shoulder-hip). Watch this video to learn how to find neutral alignment in your body. - Practice the “#1 Most Effective Core Exercise”
One of the best things you can do to expedite your healing, is to practice 360° Breathing (AKA the #1 most effective core exercise). Among numerous other benefits, 360° Breathing activates your critical deep core muscles, which is the first step to rebuilding your core strength. It also activates your body’s parasympathetic nervous system (the “rest and digest” system), which will support your body’s healing. - Incorporate Gentle Pelvic Floor Exercises
As mentioned earlier, the trauma to your abdominal muscles during a Cesarean impacts your pelvic floor as well. Begin by very gently activating your pelvic floor muscles as soon as possible following delivery. This helps increase circulation in the area to expedite healing. Then, slowly introduce the pelvic floor exercises. This does not mean doing “Kegels” as they are typically taught. Learn how to perform effective pelvic floor exercises that help you target all the muscles of your pelvic floor to develop strong, well-functioning muscles. - Consider an Abdominal Wrap or Compression Garments
Abdominal wraps, or binders, can be helpful for managing acute pain following delivery, or providing support during more strenuous activities, like going on a long walk or wearing your baby for an extended amount of time. If you choose to wear one, just be sure to avoid wrapping it too tight, as this can increase the pressure on your pelvic floor. For some helpful guidance on postpartum abdominal wraps – including when they can be useful, when they are not useful, and how to select and wear one – see this post on Should you use a postpartum belly wrap?Alternatively, compression garments – like those from SRC Health — can also be helpful in managing pain and providing support. Choose which option feels the most comfortable to you. Just remember that binders and compression garments are not meant to be worn ALL day for an extended period. They should be use temporarily to manage pain. You don’t want to start relying more on these items for support than your own body awareness and deep core strength.
Get More Information
For 10 additional recovery strategies, along with guidance on scar mobilization work, and tips for preparing for a planned Cesarean, grab our guide below for just $27. In this guide, you will learn:
- What Happens During the Procedure
- Types of Cesarean Births and Common Reasons for Each
- Typical Procedure vs. Family-Centered (Gentle) Cesarean
- 15 Recovery Strategies
- Scar Mobilization Process & Techniques
- Tips to Prepare for a Planned Cesarean

Sources
(1) Gibbons, L., Belizán, J.M., Lauer, J.A., Betrán, A.P., Merialdi, M., & Althabe, F. (2010). The Global Numbers and Costs of Additionally Needed and Unnecessary Caesarean Sections Performed per Year: Overuse as a Barrier to Universal Coverage. World Health Report, Background Paper, 30.
(2) Broadbent, E. & Koschwanez, H.E. (2012). The Psychology of Wound Healing. Current Opinion in Psychiatry, Vol 25 (2), 135-140.