The pelvic floor (PF) is an unsung hero of the body that tends to get ignored until something goes wrong “down there.” Unfortunately, during pregnancy, the physical and physiological changes to the body often alter the function of the PF, and lead to pelvic floor dysfunction. One example of pelvic floor dysfunction is Pelvic Organ Prolapse (POP). In this article, we’ll help you understand what POP is, the potential causes, and treatment options.
But first, let’s begin with a basic understanding of your pelvic floor.
Understanding Your Pelvic Floor
Your pelvic floor is comprised of three layers of muscles (14 muscles in total), which form a sling at the bottom of your core (or the “floor of the core”). Yes — your pelvic floor muscles are critical core muscles, even though they are often not the first to come to mind when we think of the core.
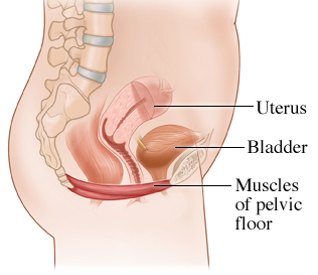
A well-functioning pelvic floor is responsible for:
- Supporting your pelvic organs: uterus, bladder, rectum
- Helping to stabilize your spine and pelvic-hip region
- Controlling continence (making sure you pee when you want to, and don’t pee when you don’t want to)
- Aiding in sexual response and satisfaction
- Assisting in guiding the baby out during delivery
What is Pelvic Organ Prolapse?
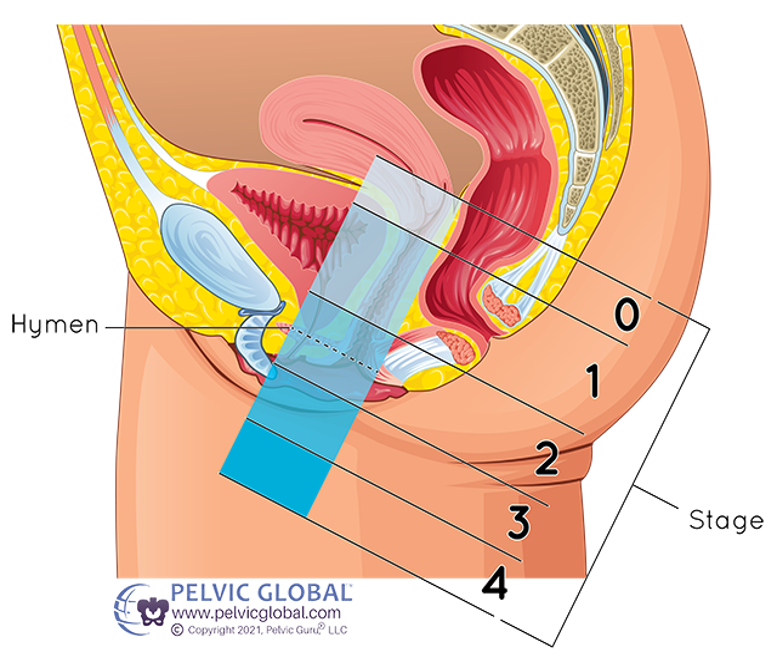
POP is when one or more of the pelvic organs (bladder, rectum, or uterus) descends lower than its normal position in the pelvic cavity. There are 4 grades of POP, as you can see in the diagram below. The higher the grade, the more severe the prolapse. Grade 0 = no prolapse while Grade 4 is when one (or more) of the pelvic organs descends so low that it can protrude through the vagina or rectum. This case may require surgery, but it is rare.

What are the Symptoms of POP?
Depending on the which organ is affected, different symptoms can be experienced. According to pelvic floor physical therapist, Dr. Mukta Chauhan, common symptoms she sees are:
- Heaviness, pressure, or ache in the groin area
- Incontinence (urinary or fecal)
- Urgency/ frequency of urine
- Hesitancy to start the stream or weak or prolonged stream
- Incomplete emptying (urinary or fecal)
- Painful intercourse
It is important to note that the severity of symptoms may not mirror the severity of organ descent (or POP grade). For example, Dr. Mukta says that she has many patients with lower grade prolapse who exhibit more severe symptoms than those with a higher grade.
What are the Potential Causes of POP?
There are several potential causes of POP. Below are some common factors that can increase the likelihood of developing it.
- Hormonal changes as you age: POP is incredibly common place in older age (Nygaard, et. al., 2004). A key reason for this is hormonal changes, which alter the soft tissues of the pelvic floor, making them less supportive.
- Childbirth: This should come as no surprise. Either delivery method — vaginal or cesarean — impacts the pelvic floor. In a vaginal birth, the pelvic floor muscles are responsible for helping to guide the baby out during delivery. However, if these muscles are underactive, or in a weakened and shortened state, this could result in increased tearing. A cesarean also traumatizes the pelvic floor muscles because the procedure involves moving the abdominal muscles, which are intricately connected to the pelvic floor. The greater the number of children one has birthed, the greater the likelihood of developing POP (Walker & Gunasekera, 2011).
- Pregnancy Alignment Shifts: During pregnancy, the growing belly tends to tip the pelvis forward into an anterior pelvic tilt (as you can see pictured below). This increases the stress on the pelvic floor muscles.

- Weak (or overwhelmed) deep core muscles: The deep core muscles of the “Core Canister” (diaphragm, transverse abdominis, and pelvic floor) help regulate pressure in the core (or intra-abdominal pressure). If these muscles are weak — or overwhelmed from the stresses of pregnancy — they cannot regulate pressure as well, which thereby increases the stress on the pelvic floor.
- Breath-holding upon exertion: During exertion, holding your breath can add more pressure to the abdominal and pelvic cavities, placing excessive pressure downward onto the pelvic floor. One example of this is the “Valsalva maneuver,” which is sometimes used as a strategy to generate more force when lifting very heavy loads (this is also a key reason many powerlifters also experience various forms of pelvic floor dysfunction). Another example of breath-holding upon exertion is bearing down on the toilet during a difficult bowel movement. Unfortunately, constipation is a common side effect during pregnancy, but consistent bearing down puts tremendous downward pressure on the pelvic floor.
- Chronic core engagement: Whether intentional or not, many of us maintain chronic tension in our core muscles (for aesthetics, or because we mistakenly think more engagement results in a stronger core). However, chronic core engagement increases pressure in the core, especially the downward pressure onto the pelvic floor.
Treatment Options for POP
Ideally, pelvic floor physical therapy should be the first line of treatment, and may include specific pelvic floor and core exercises as well as the use of a pessary — a device that helps provide internal support for the prolapsed organ. You can use this PT Locator provided by APTA (American Physical Therapy Association) Pelvic Health to find a qualified Women’s Health PT near you.
In addition, focus on the following strategies to help alleviate excess stress on your pelvic floor:
- Focus on moving in neutral alignment
- Avoid breath-holding upon exertion and chronic core engagement. Follow these tips to to reduce constipation if needed.
- Master the #1 most effective core exercise, or 360˚ Breathing. This style of breathing activates the deep “Core Canister” muscles to help regulate the pressure in your core.
- Strengthen your pelvic floor muscles by working them through a full range of motion. For guidance on how to do this, watch this video on how to perform Pelvic Floor Activations (PFAs).
- To help with comfort, support, and managing continence, consider a prolapse-specific compression garment like this one from SRC Health. We love how this garment provides support and comfort, and helps manage continence, without increasing intra-abdominal pressure.
Additional Support
- If you have painful symptoms, consider wearing a compression garment. We love the range from SRC Health, which offers high-quality garments to wear under and over your bump (use code PRONATAL10 for 10% off).
- For programs and services to help you exercise safely and effectively during pregnancy, check out our training programs & services.
- If you are a health & fitness pro interested in coaching pre & postnatal clients, explore our ProNatal Education & Certification.
Post Contributor
Dr. Mukta Chauhan, DPT, OCS, WCS is one of the few physical therapists in the country with a double board certification in orthopedics and women’s health. Because of this dual training, Dr. Mukta understands the delicate interplay between neurophysiology, biomechanics, musculoskeletal, fascial and organ systems and their combined contribution to a person’s overall wellbeing. She is a firm believer in addressing health from a bio-psycho-social perspective, because we aren’t just our tissues. The whole person is at the center of her practice. She lives and practices in New York City. Connect with her on IG @thepelvic.connection.
Sources
Nygaard, I., Bradley, C., & Brandt, D. (2004). Pelvic organ prolapse in older women: prevalence and risk factors. Obstetrics & Gynecology, 104(3), 489-497.
Walker, G. J., & Gunasekera, P. (2011). Pelvic organ prolapse and incontinence in developing countries: review of prevalence and risk factors. International urogynecology journal, 22(2), 127-135.
Affiliate Notification
The SRC link is an affiliate link. We may earn a commission from purchases made through this link, but we only endorse companies that we have vetted and believe in.