This is the last post in our 3-part series. In our first post, Childbirth Preparation Overview, we focused on helping you understand what actually happens during labor. In our second post, Stage 1 Breakdown, we provided strategies for managing through Stage 1 Labor — from energy management, to position variety, to mindset tips. Now we are ready to move on to helping you prepare for Stage 2 Labor (the “pushing” stage). The tips below can help make your pushing more effective, reduce the duration of the pushing stage, and minimize stress to your body (especially your pelvic floor). We will discuss the following three elements of pushing: timing, position, and technique.
Pushing Timing
Once the cervix has dilated fully to 10 cm, typically the medical professional will instruct you to begin pushing almost immediately. This is known as managed pushing (or instructed pushing). However, you may not feel quite ready to push just because you are 10 cm dilated. That is because there is often a period of quietude that exists in between Stages 1 & 2 – a phase that does not get attention in traditional medical circles – in which contractions may slow or stop altogether. This happens to allow the baby more time to perform its complex series of cardinal movements so that it is truly ready to be pushed out.
If you can take these quiet moments to breathe deeply, re-center yourself, and prepare physically and mentally for the final “push” (pardon the pun), then the process can be much more efficient. This type of internally derived know-how is called instinctive pushing (or physiologic pushing). All you need to do is listen to your body, then begin pushing only when you feel the uncontrollable urge to do so. Of course, to do this, you need to be in an environment that is supportive of allowing you to take this time. This is why it is so important to find a medical provider (early on) who aligns with your needs and values.
Pushing Position
Now that we’ve discussed when to push, let’s discuss the various positions to push in. The most common birthing position today in a hospital setting is reclining with legs bent and knees in stirrups, like below:

This position enables doctors to have access to see, maneuver, and (if necessary) perform interventions. However, if we take a brief look at how our more “primitive” ancestors gave birth — when they were left to their own devices to do what felt natural for their bodies — the most common positions were standing (supported), squatting, or hands-and-knees because these positions offered the advantage of gravity’s downward pull.
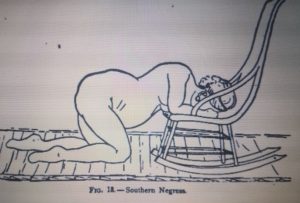
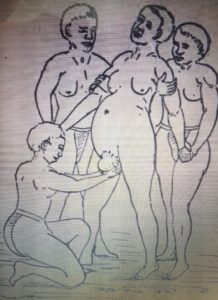

For more information on effective pushing positions, check out this post on Questioning Childbirth Positions. It takes you through a step-by-step process to find the position that creates the greatest space in your pelvis for baby to pass through. You might be quite surprised by what position this actually is!
Pushing Technique
Finally, let’s discuss the actual technique of pushing. Traditionally, many doctors will typically tell you to “hold your breath” or “bear down” and push. However, this strategy of breath-holding upon exertion spikes the pressure inside your core, which can lead to greater issues with Diastasis Recti and Pelvic Floor Dysfunction. It can also reduce oxygenation to the baby and result in potential heart rate deceleration, especially if used as your only pushing strategy for an extended period. Moreover, when you bear down and tense your body, this doesn’t exactly make it easy for your baby to pass through.
To help you learn to push in a safer, and more efficient, manner, check out this piece on Preparing to Push. It will walk you through a three step process that begins with mastering proper breathing mechanics, then helps you establish control of your pelvic floor muscles through a full range of motion, then finally helps you master a pushing strategy that does not involve breath-holding.
Want Additional Resources?
For additional resources to help you exercise safely and effectively during pregnancy, explore our training programs and services. You’ll find a variety of offerings tailored to different needs — from education, to self-guided programs, to the ability to work with an expert coach.
Or, if you’re a health & fitness pro interested in coaching pre & postnatal clients, check out our ProNatal Education & Certification.
Sources:
Engelmann, G.J. (1882). Labor Among Primitive Peoples. St. Louis: JH Chambers.
Lemos, A., Dean, E., & Andrade, A.D. (2011). The Valsalva maneuver duration during labor expulsive stage: repercussions on the maternal and neonatal birth condition. Brazilian Journal of Physical Therapy, 15(1), 66-72.
